A novel class of drugs for the treatment of fibrotic diseases
Fibrosis: a pathological wound healing process in which connective tissue replaces normal parenchymal tissue;
As the process continues unchecked, this leads to considerable tissue remodelling and deposition of connective tissue
The result is interference or complete inhibition and loss of function of the organ affected
Platform Technology
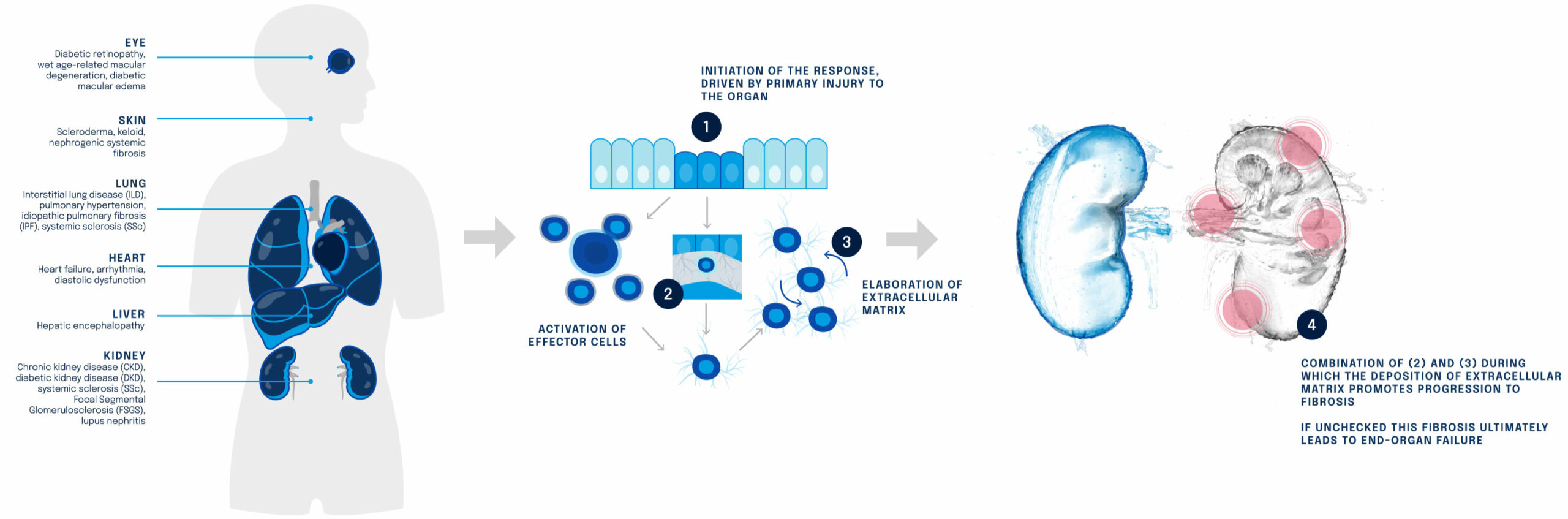
Figure: Fibrosis is a highly dynamic process that can be arrested with precision medicine
The fibrosis mechanism of action has now been characterised, where this mechanism contributes to many serious and life-limiting fibrotic diseases, including Chronic Kidney Disease (CKD), Systemic Sclerosis (SSc), Focal Segmental Glomerulosclerosis (FSGS) and others.
Our research has identified a novel biologic target in the fibrosis mechanism as a defined G protein-coupled receptor (GPCR). This GPCR is silent in healthy tissue but activated following injury or disease. Evidence demonstrates the role this GPCR has on multiple downstream pathways causing inflammation and fibrosis.
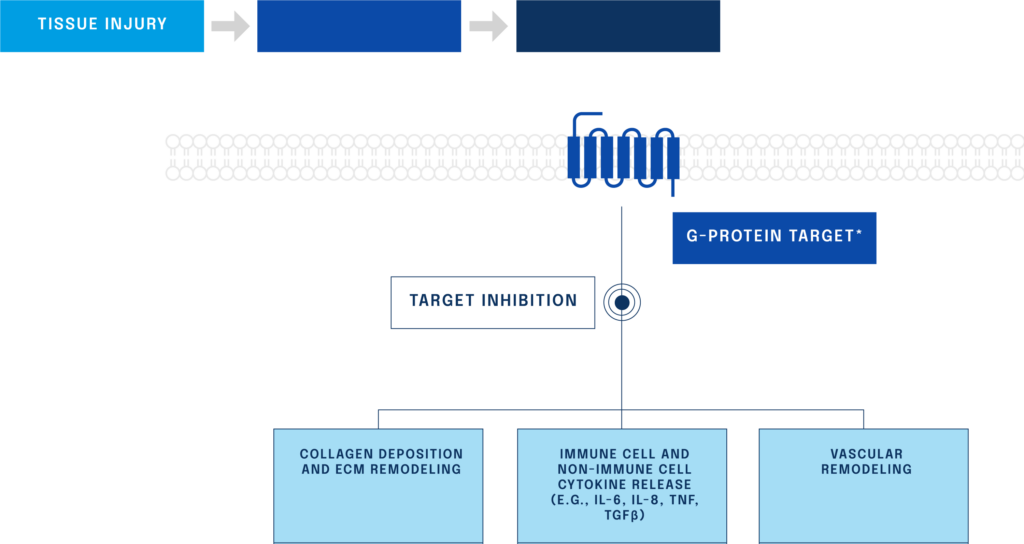
Figure: Inhibition of the novel target affects multiple pathways post-tissue injury
Developing innovative precision therapies for fibrosis
The new class of drugs being developed by OccuRx are potent and selective antagonists of this GPCR target, inhibiting fibrotic and inflammatory pathways.
These GPCR inhibitors comprise a platform of structurally analogous candidate therapies, designed to offer new treatment options for patients with various fibrotic diseases.
It is hypothesized that the GPCR target, which is activated due to disease or injury and that leads to fibrosis, can be inhibited by administration of these novel drugs. If successful, this could stop the fibrosis in patients, potentially slowing the rate of disease progression.
The research conducted on the new candidate therapies being developed by OccuRx includes efficacy studies, where treatment with these new drugs leads to a positive impact on organ function in multiple models of fibrotic diseases.
Fibrosis in Scleroderma
(Systemic Sclerosis)
Scleroderma (including systemic sclerosis, SSc) is a rare and potentially life-threatening autoimmune disorder characterised by inflammation (thickening) and fibrosis (hardening/scarring) of the skin and other organs.
Fibrosis in Chronic Kidney Disease, including Diabetic Kidney Disease
Chronic kidney disease (CKD) is a term that encompasses all degrees of decreased kidney function, from mild or moderate disease to severe and end organ failure.
Fibrosis in Focal Segmental Glomerular Sclerosis
Focal segmental glomerulosclerosis is one of the many kidney conditions described under the umbrella of glomerulonephritis (inflammation of the kidney), which can lead to chronic kidney disease. FSGS is a condition that results in hardening or thickening of the glomeruli, which act as filters inside the nephrons of the kidney.
Fibrosis in Ocular
Diseases
Fibrosis is observed in multiple eye diseases, including diabetic retinopathy (DR) and age-related macular degeneration (AMD), where the deposition of scar tissue is irreversible, impacting vision and, in the case of DR, can ultimately lead to blindness.
Breakthrough science in the most advanced therapeutic program for this receptor
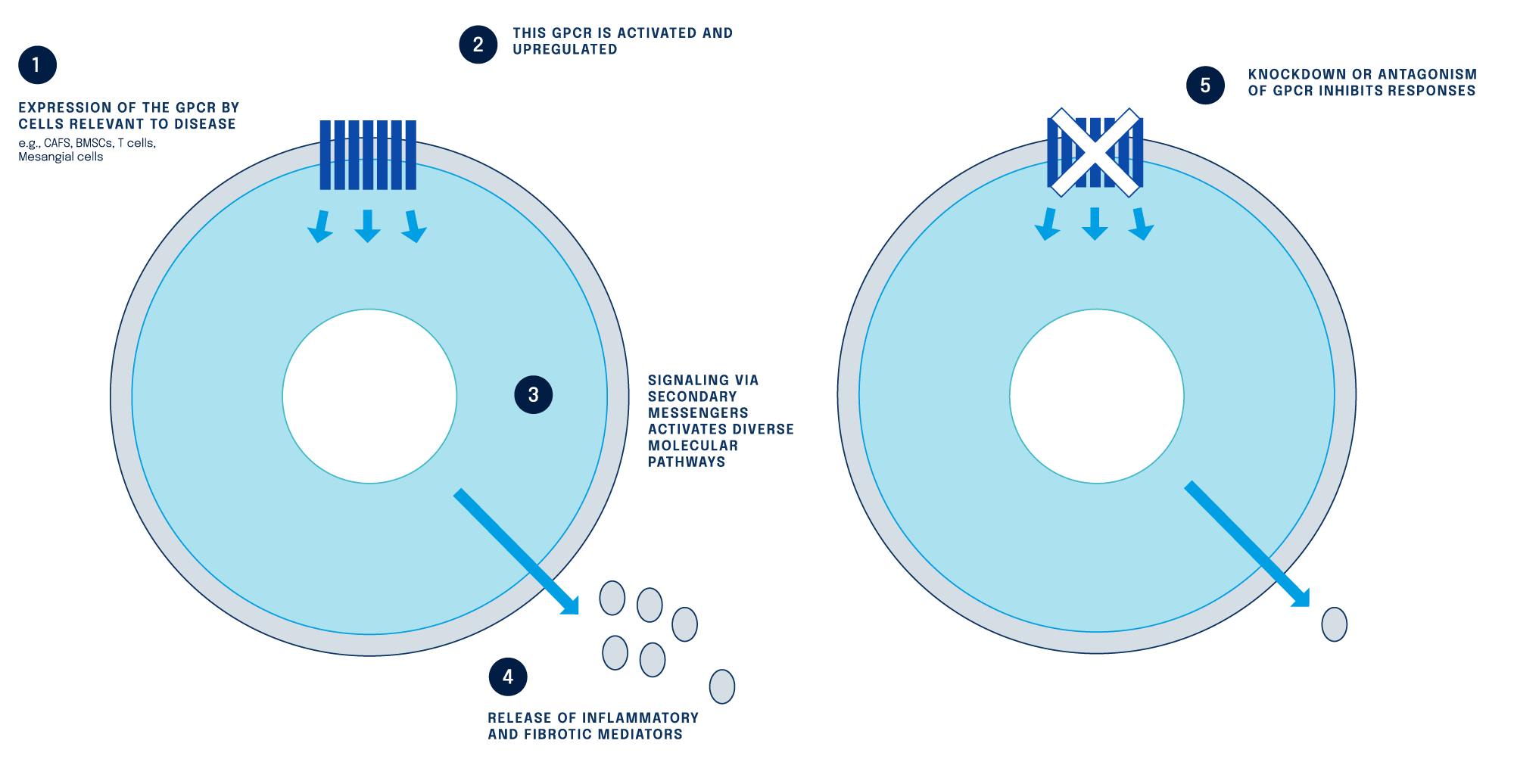
Figure: The fibrosis mechanism of action has been characterised
Extensive pre-clinical studies, conducted by our team in addition to collaborations with world-leading experts, have now identified a biologic pathway and protein target which is critical to the fibrosis pathway.
In response to injury to body tissues or trauma caused by disease (including organs), a specific G protein-coupled receptor (GPCR) becomes activated. This activated GPCR then triggers multiple downstream processes, including inflammatory responses (immune cell and non-immune cell cytokine release), local changes to blood vessel structures (vascular remodelling) and laying down of excess fibrotic or scar tissue (collagen deposition and extracellular matrix remodelling).
As an example, fibrosis in the kidney can occur for a range of reasons, including as a result of diabetes, certain cardiovascular or metabolic diseases. The fibrosis leads to a decline in renal function over time, reducing the body’s ability to effectively filter out toxins and waste products from the bloodstream. The compounding effect drives the progression of chronic kidney disease, and then to end-stage renal disease (ESRD) with an eventual requirement for dialysis or kidney transplantation.
Our pre-clinical studies have shown that inhibiting this activated GPCR can either stop or reduce the fibrotic response, and this in turn results in improved clinical outcomes.
The new class of molecules (including FT011, OCX063 and next-generation candidates) have been designed and developed as potent and selective antagonists to the GPCR target, inhibiting anti-fibrotic and anti-inflammatory pathways.
Our research in efficacy models has shown positive impact on organ function following treatment with these new therapies.
More information on the progress and the diseases being studied is described in the Pipeline section.
Disclaimer
All of the candidate drugs described on this site are investigational products which have not received marketing authorization or approval by any regulatory agency, including the US Food and Drug Administration, the European Medicines Agency, or the Australian Therapeutic Goods Agency. The investigational drug products are undergoing clinical studies to evaluate the safety and effectiveness in humans.
